Introduction
Imagine standing before the mirror, yearning for a reflection that embodies your inner beauty, yet grappling with the shadows of uncertainty that accompany breast augmentation. This transformative journey, while promising, carries the risk of complications such as implant rupture, which can lead to significant pain and distress.
What if the very source of your confidence became a source of concern, casting a shadow over your self-assurance? This article invites you to join us as we explore the nuances of breast implant rupture pain, from the differences between saline and silicone implants to the diagnostic methods and treatment options that can empower you on your journey to beauty and well-being.
Define Breast Implant Rupture: Importance and Implications
Imagine the moment you realize that your journey toward beauty and confidence may be jeopardized by breast implant rupture pain from your augmentation device. A tear or hole in the outer shell of a mammary augmentation device can occur in both saline and silicone versions, leading to distressing implications.
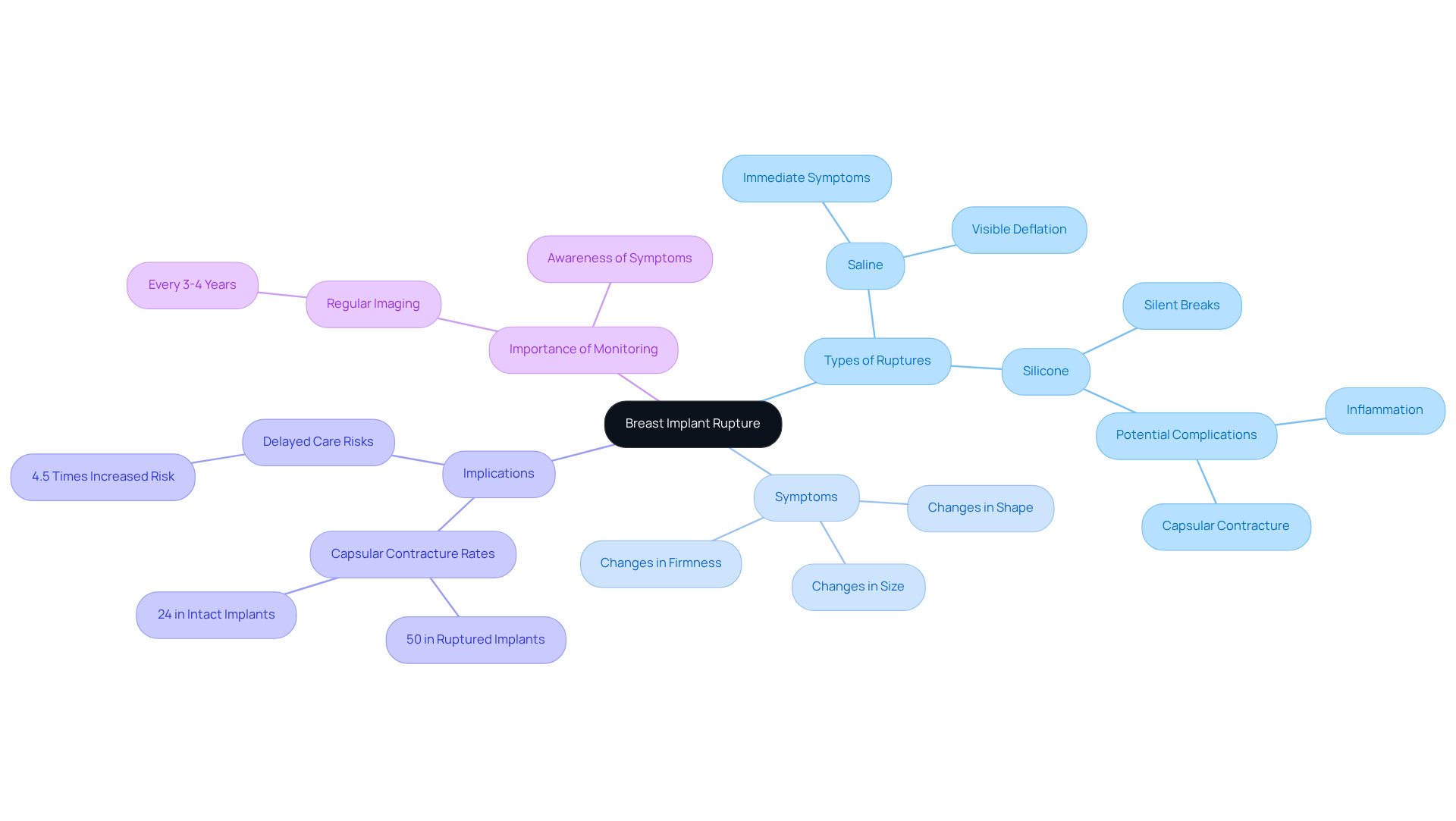
When a saline implant ruptures, the saline solution leaks out, resulting in a visible deflation of the breast. This often prompts immediate concern as the change in chest shape and size becomes apparent. Conversely, silicone breaks can be more insidious, often referred to as ‘silent breaks.’ These may not present immediate symptoms, allowing the silicone gel to leak into surrounding tissue, potentially causing complications such as inflammation or capsular contracture – the hardening of tissue around the device.
Understanding the implications of breast augmentation failure, including breast implant rupture pain, is crucial for anyone on this journey. Research indicates that delayed care following a rupture can elevate the likelihood of capsular contracture by 4.5 times, underscoring the importance of regular monitoring and awareness of symptoms. A 2026 Danish study revealed that ruptured implants had a 50% rate of capsular contracture compared to just 24% in intact implants.
It is vital for patients to recognize the signs of a rupture – changes in shape, size, or firmness – and to seek the expertise of a board-certified plastic surgeon at the first hint of breast implant rupture pain. This proactive approach not only safeguards your health but also empowers you to embrace your beauty with renewed confidence.
Identify Symptoms of Breast Implant Rupture: Saline vs. Silicone
Picture a moment when you glance in the mirror, only to notice an unsettling change in your reflection-this could be the first sign of an implant rupture. Identifying the symptoms of breast implant rupture pain is crucial for timely intervention, as the signs can differ significantly between saline and silicone implants. Understanding these differences is essential for patients seeking to maintain their beauty and confidence.
Saline Implants: Common symptoms include a sudden deflation of the breast, resulting in a noticeable decrease in size, visible rippling or distortion of the chest shape, and tenderness or discomfort in the chest area. This discomfort may arise due to loss of shape and sagging skin. Patients experiencing saline breaks are advised to avoid aspirin and ibuprofen, as these blood thinners can delay scheduling replacement surgery, potentially prolonging anxiety and uncertainty.
Silicone Implants: Symptoms may include changes in breast shape or size without visible deflation, often referred to as ‘silent ruptures.’ These may not present immediate symptoms, making regular MRI screenings recommended starting 5-6 years after placement. Dr. Golshani emphasizes the importance of proactive monitoring to ensure peace of mind. Other symptoms may include firmness or swelling in the breast, which can develop gradually, leading to irritation in surrounding tissues. Pain or tenderness may occur, particularly breast implant rupture pain, if the silicone has leaked into surrounding tissues, potentially causing localized reactions such as inflammation or silicone granulomas. Ruptured silicone devices pose greater health risks and should be removed as soon as possible.
Recognizing these symptoms early can mean the difference between a simple solution and a complicated journey. Engaging in open conversations with your healthcare provider can illuminate the path to timely intervention and peace of mind, diminishing the likelihood of complications linked to ruptured devices. It is also crucial to recognize that mammary enhancements usually endure 10-15 years. Understanding the factors of failure, such as natural deterioration, trauma, or surgical harm, can further assist in preserving mammary health. Embracing knowledge about your implants not only empowers you but also safeguards your journey toward beauty and confidence.
![]()
Diagnose Breast Implant Rupture: Methods and Procedures
Imagine the unease that accompanies the thought of breast implant rupture pain, a concern that weighs heavily on the minds of many women seeking beauty and confidence. Diagnosing breast implant rupture pain involves several methods and procedures to confirm the condition, each designed to alleviate anxiety and provide clarity.
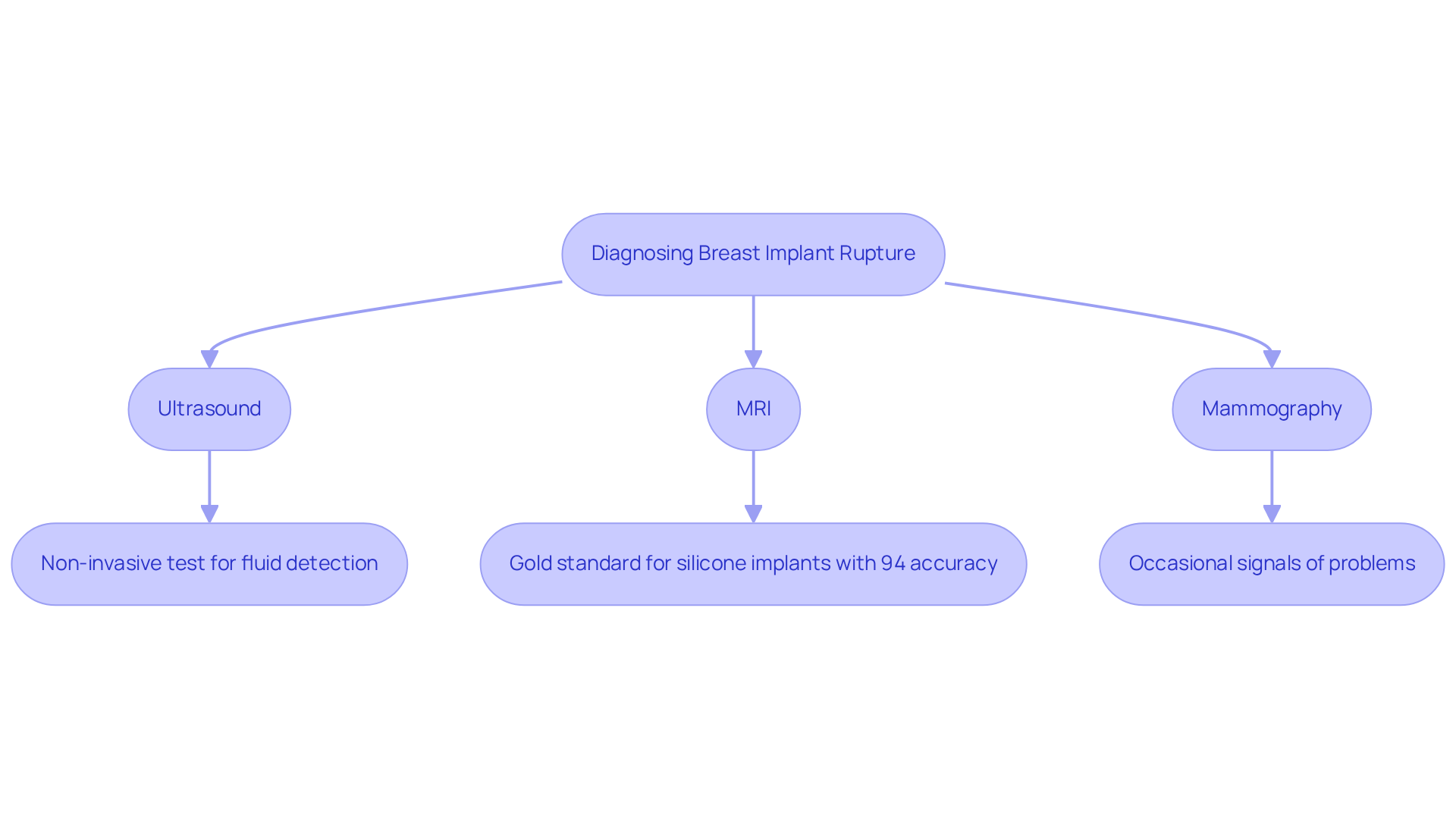
A compassionate evaluation by a skilled surgeon can reveal the subtle signs of rupture, offering reassurance in a moment of uncertainty. Among the first steps in this journey is an ultrasound, a gentle and non-invasive test that brings peace of mind to younger patients. This method effectively detects fluid around the device, making it a quick and safe choice for routine screening.
For those with silicone implants, an MRI is considered the gold standard for diagnosing breast implant rupture pain. This advanced imaging technique can identify silent ruptures by highlighting changes in the structure and surrounding tissue. Studies indicate that MRI boasts a remarkable 94% accuracy rate in detecting ruptured devices, significantly surpassing ultrasound.
While mammography may not be as sensitive as MRI, it can occasionally signal problems with chest enhancements, serving as an additional resource in the diagnostic process. By familiarizing yourself with these diagnostic methods, you not only prepare for your medical appointments but also embrace the journey toward clarity and reassurance.
Explore Treatment Options for Breast Implant Rupture: Surgical and Non-Surgical Solutions
Imagine the moment when a cherished symbol of beauty and confidence suddenly falters, leaving one to grapple with uncertainty and concern. In such instances, a range of treatment options awaits, each tailored to restore both form and confidence.
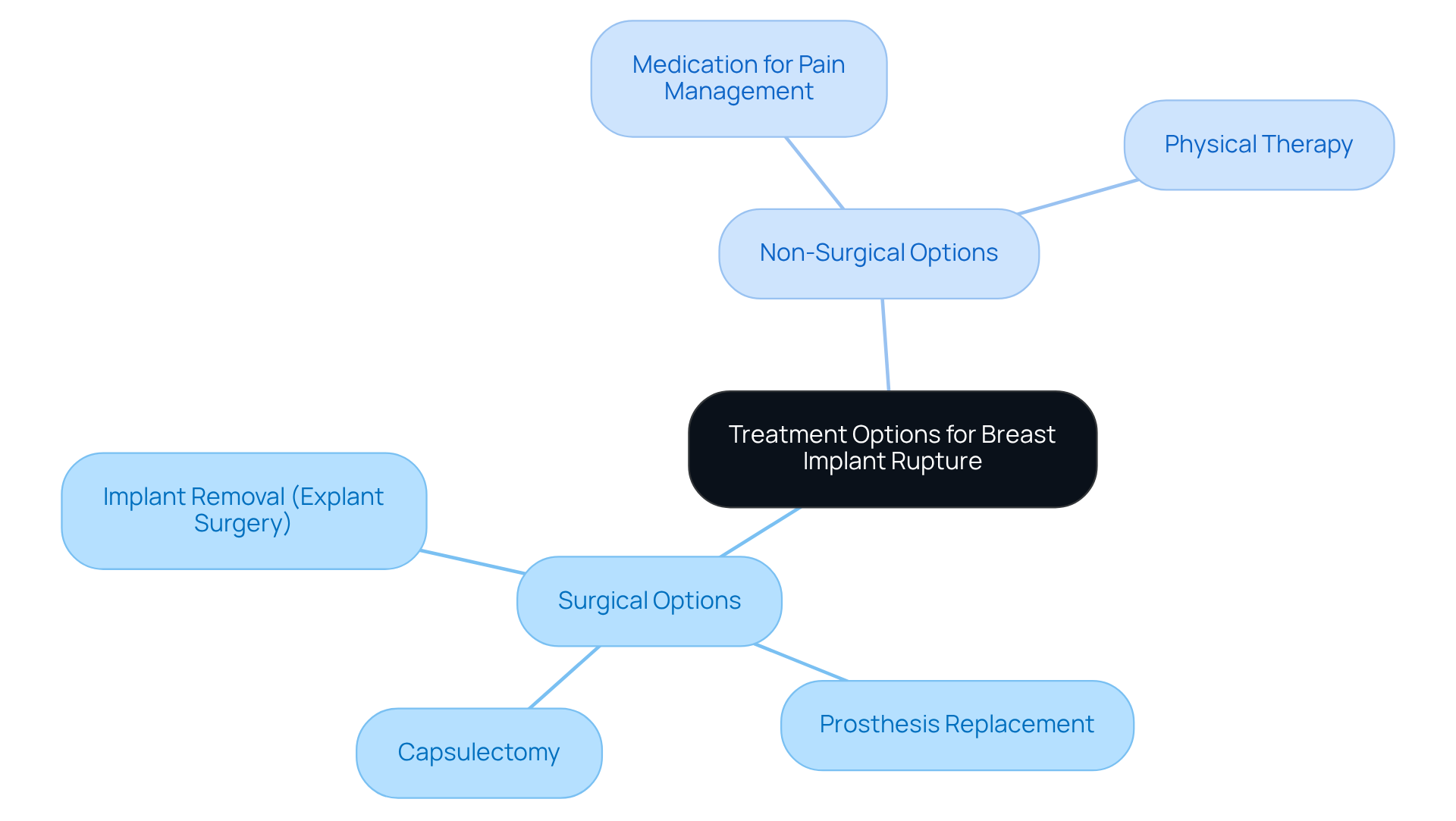
Surgical Options: The journey often begins with Implant Removal (Explant Surgery), a pivotal step in reclaiming one’s sense of self, especially for those with saline implants. Here, the surgeon delicately extracts the damaged device, addressing any surrounding tissue concerns to ensure a smooth recovery. Following this, many patients opt for Prosthesis Replacement, allowing for immediate restoration of breast volume and shape during the same surgical session. If scar tissue has developed around the implant, a Capsulectomy may be necessary, removing the scar tissue to prevent complications in future surgeries and enhance overall outcomes.
While surgical intervention is frequently required, some Non-Surgical Options can assist in managing symptoms or complications. Medication for pain management and anti-inflammatory relief can effectively alleviate breast implant rupture pain, helping patients cope during the recovery process. Additionally, Physical Therapy may prove advantageous in improving mobility and alleviating discomfort in the chest area, especially following surgery.
By understanding the available options, you can embark on a journey toward renewed confidence and beauty, transforming a moment of distress into an opportunity for empowerment. With more than 300,000 breast augmentations performed annually in the U.S., awareness of potential complications and available solutions is crucial for maintaining both physical health and psychological satisfaction.
Conclusion
Imagine the moment when a cherished symbol of beauty and confidence suddenly falters, leaving one to grapple with uncertainty and concern. Understanding breast implant rupture is essential for anyone considering or currently undergoing breast augmentation. The pain and complications associated with a rupture can significantly impact one’s confidence and well-being. Recognizing the symptoms, knowing the diagnostic methods, and exploring treatment options are crucial steps in managing breast implant rupture effectively.
Key insights from the article highlight the differences between saline and silicone implants, emphasizing the importance of early detection and intervention. Symptoms such as sudden deflation for saline implants or silent ruptures for silicone implants necessitate proactive monitoring and communication with healthcare providers. Diagnostic methods like ultrasounds and MRIs play a vital role in confirming ruptures, while treatment options range from surgical removal and replacement to non-surgical pain management.
Awareness of potential complications and timely action can transform a distressing situation into an opportunity for recovery and renewed confidence. By embracing this knowledge, you not only protect your physical health but also embark on a profound journey toward renewed beauty and self-assurance.
Frequently Asked Questions
What is breast implant rupture?
Breast implant rupture is defined as a tear or hole in the outer shell of a mammary augmentation device, which can occur in both saline and silicone implants.
What happens when a saline implant ruptures?
When a saline implant ruptures, the saline solution leaks out, resulting in a visible deflation of the breast, which can cause immediate concern due to the change in shape and size.
How do silicone implant ruptures differ from saline ruptures?
Silicone implant ruptures can be more insidious, often referred to as ‘silent breaks.’ They may not present immediate symptoms, allowing the silicone gel to leak into surrounding tissue, potentially causing complications such as inflammation or capsular contracture.
Why is it important to understand the implications of breast implant rupture?
Understanding the implications is crucial because delayed care following a rupture can significantly increase the risk of complications, such as capsular contracture, which can be 4.5 times more likely with delayed treatment.
What does research indicate about capsular contracture rates in ruptured vs. intact implants?
A 2026 Danish study found that ruptured implants had a 50% rate of capsular contracture compared to just 24% in intact implants.
What signs should patients look for to recognize a breast implant rupture?
Patients should look for changes in shape, size, or firmness of the breast as potential signs of a rupture.
What should someone do if they suspect a breast implant rupture?
It is important to seek the expertise of a board-certified plastic surgeon at the first hint of breast implant rupture pain to safeguard health and address any issues promptly.
List of Sources
- Define Breast Implant Rupture: Importance and Implications
- Breast Implant Rupture and Capsular Contracture: What Every Patient Should Know in 2026 – Orange County Plastic Surgery (https://orangecountyplasticsurgery.com/breast-implant-rupture-and-capsular-contracture-what-every-patient-should-know-in-2026)
- Risks of Breast Implants (https://fda.gov/medical-devices/breast-implants/risks-and-complications-breast-implants)
- Breast Implants: What Happens If They Rupture? (https://fortesmd.com/blog/breast-implants-what-happens-if-they-rupture)
- Breast Implant Rupture Rates In 2026: FDA Data Shows Less Than 1% Risk With Modern Implants – Perfect Doctors Clinic (https://perfectdrs.com/breast-implant-rupture-rates-in-2026-fda-data-shows-less-than-1-risk-with-modern-implants)
- Identify Symptoms of Breast Implant Rupture: Saline vs. Silicone
- Ruptured vs. Leaking Breast Implants: What You Need To Know (https://nwplasticsurgery.com/ruptured-vs-leaking-breast-implants)
- How To Tell If Your Breast Implant Has Ruptured (https://drsteeleplasticsurgery.com/blog/how-to-tell-if-your-breast-implant-has-ruptured)
- Breast Implant Rupture: Signs and Treatments (https://breastcancer.org/treatment/surgery/breast-reconstruction/corrective-reconstruction/implant-rupture)
- Possible complications of silicone breast implants (https://mayoclinic.org/healthy-lifestyle/womens-health/expert-answers/breast-implants/faq-20058454)
- 4 Signs Of A Ruptured Breast Implant | Dr. Michael Brucker | Brucker Plastic Surgery (https://drbrucker.com/blog/4-signs-of-a-ruptured-breast-implant)
- Diagnose Breast Implant Rupture: Methods and Procedures
- Abstract PS4-04-07: Improved Diagnostic Accuracy for Breast Implant Rupture Through Strain Elastography – Results of a User-Based Evaluation Using Standardized Image Sets (https://aacrjournals.org/clincancerres/article/32/4_Supplement/PS4-04-07/773696)
- New Tool May Help Predict Breast Implant Rupture Risk (https://healthmanagement.org/c/imaging/news/new-tool-may-help-predict-breast-implant-rupture-risk)
- How to Detect Ruptured Breast Implants (https://drcassileth.com/how-to-detect-ruptured-implants)
- MRI Is Most Accurate Test for Detecting Ruptured Silicone Breast Implants (https://plasticsurgery.org/news/press-releases/mri-is-most-accurate-test-for-detecting-ruptured-silicone-breast-implants)
- What’s the best approach to imaging of breast implant rupture? (https://auntminnieeurope.com/clinical-news/article/15658270/whats-the-best-approach-to-imaging-of-breast-implant-rupture)
- Explore Treatment Options for Breast Implant Rupture: Surgical and Non-Surgical Solutions
- Breast Implant Rupture: Signs and Treatments (https://breastcancer.org/treatment/surgery/breast-reconstruction/corrective-reconstruction/implant-rupture)
- Los Angeles Breast Implant Rupture Repair | Beverly Hills Corrective Breast Surgery (https://kamrezzadehmd.com/breast-implant-rupture-repair)
- Don’t Panic: A Surgeon’s Expert Advice on Getting Rid of Ruptured Breast Implants Safely | Marin Aesthetics (https://marinaesthetics.com/getting-rid-of-ruptured-breast-implants)
- Management of ruptured breast implants (https://thepmfajournal.com/features/features/post/management-of-ruptured-breast-implants)
- Ruptured or Leaking Breast Implants | What to Do Next – Dr. John Burns (https://drjohnburns.com/blogs/news/ruptured-or-leaking-breast-implants-what-to-do-next-dr-john-burns-dallas?srsltid=AfmBOopUbxbiqEjVZv2huTOGBekDQQ5QHNsyn8znlYqipa9ENK7JCC-O)

