Introduction
Breast reconstruction following a mastectomy marks a profound milestone in the journey toward reclaiming not only physical appearance but also emotional well-being. An impressive 76% of women report an enhanced body image after undergoing these transformative procedures, underscoring the critical importance of understanding the myriad reconstruction options available. Yet, the decision-making process can feel overwhelming, as patients find themselves navigating a spectrum of methods – from implants to tissue flaps – each presenting its own unique benefits and challenges.
What essential factors should individuals contemplate to ensure they select the path that harmonizes with their personal needs and aspirations?
Explore the Importance of Breast Reconstruction After Mastectomy
Surgical restoration following a mastectomy is not merely a procedure; it is a vital journey toward reclaiming both the physical beauty of the chest and the emotional well-being of individuals. Many women encounter profound psychological challenges in the aftermath of a mastectomy, grappling with feelings of loss and diminished self-esteem. Reconstruction options after mastectomy emerge as a pivotal step in this journey, allowing patients to rediscover their sense of wholeness and femininity, ultimately helping them rebuild their confidence.
Research reveals that approximately 76% of women who undergo breast reconstruction report significant enhancements in body image and overall quality of life. This underscores the importance of emotional stability, recognized as the most crucial predictor of quality of life, highlighting the essential role of emotional healing in this context. The timing of reconstruction-whether immediate or delayed-also plays a critical role in emotional recovery. Immediate breast reconstruction is associated with superior emotional outcomes, effectively alleviating feelings of distress and fostering self-esteem.
Dr. Golshani employs advanced techniques, such as the Keller Funnel and the no-touch technique, ensuring a safe and efficient procedure that minimizes risks and enhances recovery. Patients often express appreciation for the personalized care and attention they receive during consultations, where Dr. Golshani attentively listens to their aesthetic aspirations and concerns. It is equally important to address specific issues, such as breastfeeding after augmentation and the pros and cons of implant placement, as these factors significantly influence the decision-making process.
Testimonials from satisfied individuals portray his practice as a sanctuary, highlighting the nurturing environment that fosters recovery and reassurance. Therefore, it is imperative for patients to engage in thorough discussions with their healthcare providers regarding reconstruction options after mastectomy to ensure the most favorable psychological and physical outcomes.
Examine Types of Breast Reconstruction: Implants vs. Tissue Flaps
In the realm of reconstruction options after mastectomy, two primary avenues emerge: implant-based reconstruction and tissue flap reconstruction, each offering unique pathways to restoration and beauty.
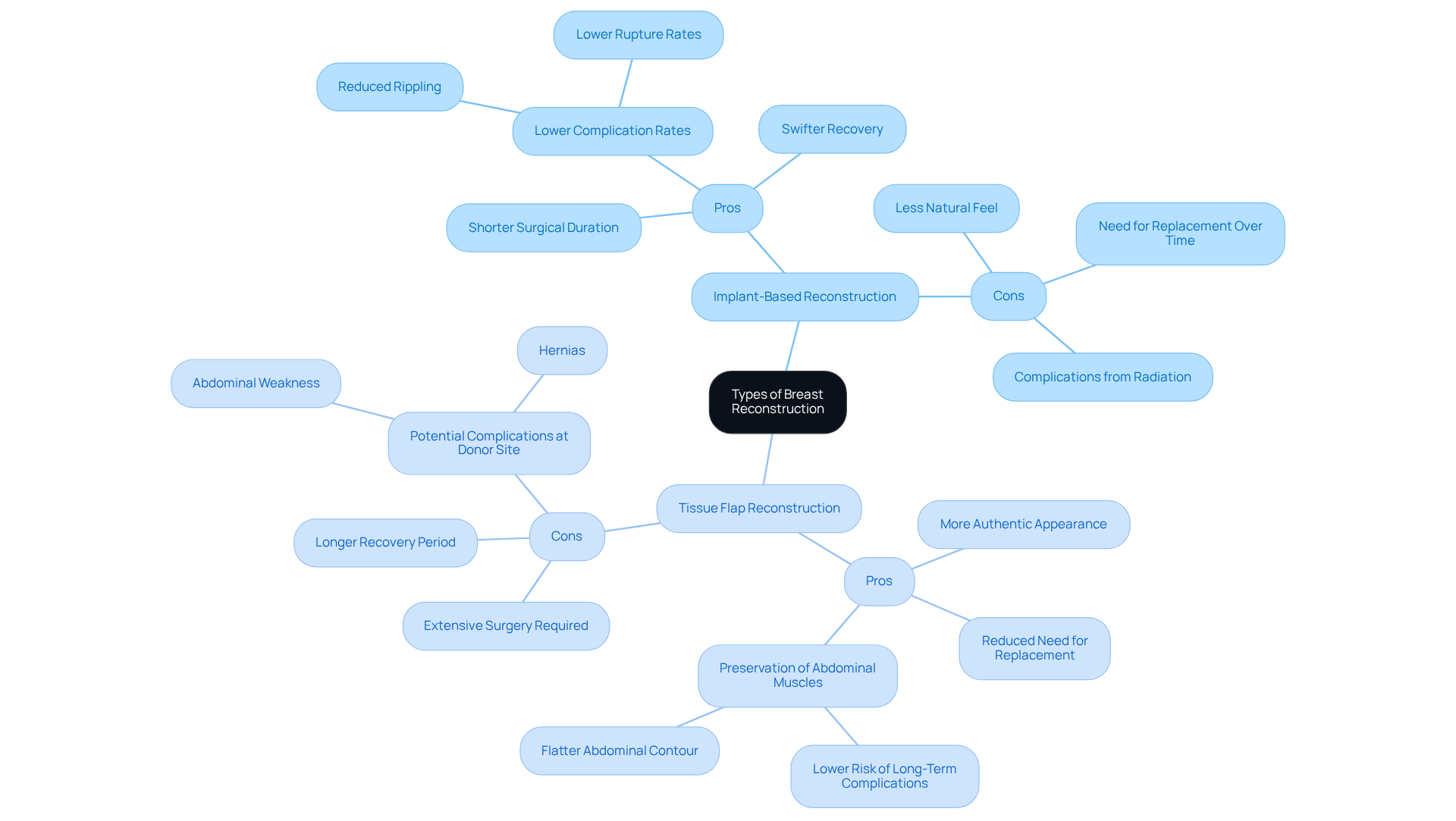
Implant-Based Reconstruction: This method involves the insertion of silicone or saline implants, artfully designed to recreate the breast’s natural shape. Often regarded as less invasive, it can be performed in a single stage or as part of a two-stage process that incorporates tissue expanders.
- Pros: This approach typically boasts a shorter surgical duration and a swifter recovery, eliminating the need for additional procedures to harvest tissue. Modern implants have demonstrated lower rates of complications, such as rippling and ruptures, compared to their predecessors.
- Cons: While implants can yield satisfactory aesthetic results, they may lack the natural feel of tissue flaps and often necessitate replacement over time, particularly in patients who have undergone radiation therapy, which can complicate the viability of the implants.
Tissue Flap Reconstruction: This technique draws upon tissue from another area of the body-be it the abdomen, back, or thighs-to sculpt a new breast.
- Pros: Flap reconstruction often results in a more authentic appearance and sensation, with the added advantage of reduced likelihood of needing replacement. Techniques such as the DIEP flap preserve abdominal muscles, mitigating the risk of long-term complications while providing a flatter abdominal contour akin to a tummy tuck.
- Cons: However, this method entails more extensive surgery and a lengthier recovery period, along with potential complications at the donor site, such as abdominal weakness or hernias.
As individuals contemplate their journey toward chest restoration, it is essential to evaluate their body type, lifestyle, and personal preferences when considering reconstruction options after mastectomy. Engaging with a qualified surgeon is paramount to discerning the most suitable approach tailored to one’s unique needs. Real-world experiences reveal that women opting for tissue flap procedures frequently report heightened satisfaction levels, particularly those who have undergone radiation, as this method tends to yield a more durable and natural outcome.
Understand the Steps Involved in the Breast Reconstruction Process
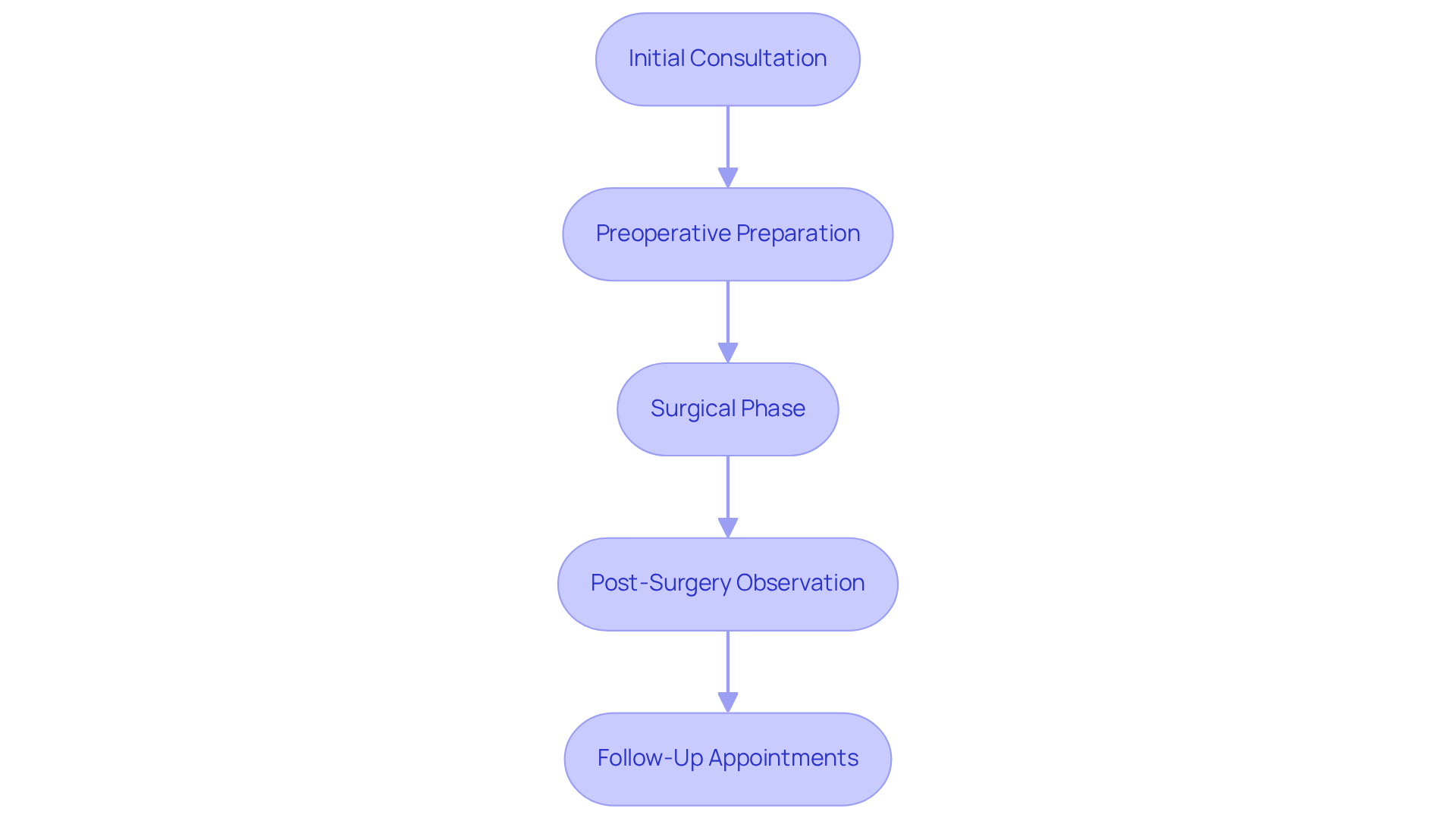
Embarking on the journey of breast reconstruction is a deeply personal experience, one that begins with a thoughtful consultation with Dr. Daniel Golshani. Here, individuals share their aspirations, medical histories, and the various reconstruction options after mastectomy that are available. This initial meeting is not merely procedural; it is a vital opportunity to set expectations and explore the unique pathways tailored to each individual. Dr. Golshani approaches every case with the utmost respect, ensuring that all concerns are addressed with care and ample time. Patients are encouraged to engage actively, asking questions and voicing their thoughts, fostering a collaborative atmosphere.
As the journey unfolds, preoperative preparation becomes essential. Patients may undergo imaging tests to assess their specific needs, receiving tailored instructions on how to prepare for surgery, including dietary adjustments and medication considerations. Research underscores the importance of preoperative imaging, which can significantly enhance surgical planning and outcomes, evidenced by a notable increase in procedural volume since 2000.
The surgical phase marks a pivotal moment in this transformative journey. There are reconstruction options after mastectomy that may occur immediately following the procedure or at a later date, depending on individual circumstances. Dr. Golshani employs techniques that may include implant placement or tissue flap surgery, each customized to the patient’s anatomy and preferences. His approach ensures that individuals feel both comfortable and informed throughout the process, fostering a sense of empowerment.
Post-surgery, individuals enter a phase of observation, where any potential complications are monitored closely. Comprehensive pain management strategies and detailed care instructions are provided, facilitating a smooth healing process. Many individuals report a swift recovery, with some returning to work within weeks, a testament to the advancements in surgical techniques. As one patient, Athaliah McPherson, beautifully articulated, ‘I am 100% happy with my results.’
Follow-up appointments play a crucial role in this journey, allowing for ongoing monitoring of healing and addressing any concerns that may arise. During these visits, discussions about further procedures, such as nipple restoration or modifications, ensure that the final results align seamlessly with the individual’s expectations. Dr. Golshani’s unwavering commitment to continuous support means that individuals can reach out to him even years after their procedure.
Moreover, the Advocate® app serves as an invaluable resource, empowering individuals to engage in meaningful discussions with their doctors and explore reconstruction options after mastectomy.
Understanding these steps not only prepares individuals for their surgical journey but also encourages active participation in their care, fostering a sense of confidence and knowledge that is essential for this transformative experience.
Navigate Recovery After Breast Reconstruction: Tips and Expectations
Recovery after breast reconstruction is a journey marked by resilience and hope, varying significantly based on the surgical approach. Yet, certain strategies can universally aid patients during this critical phase:
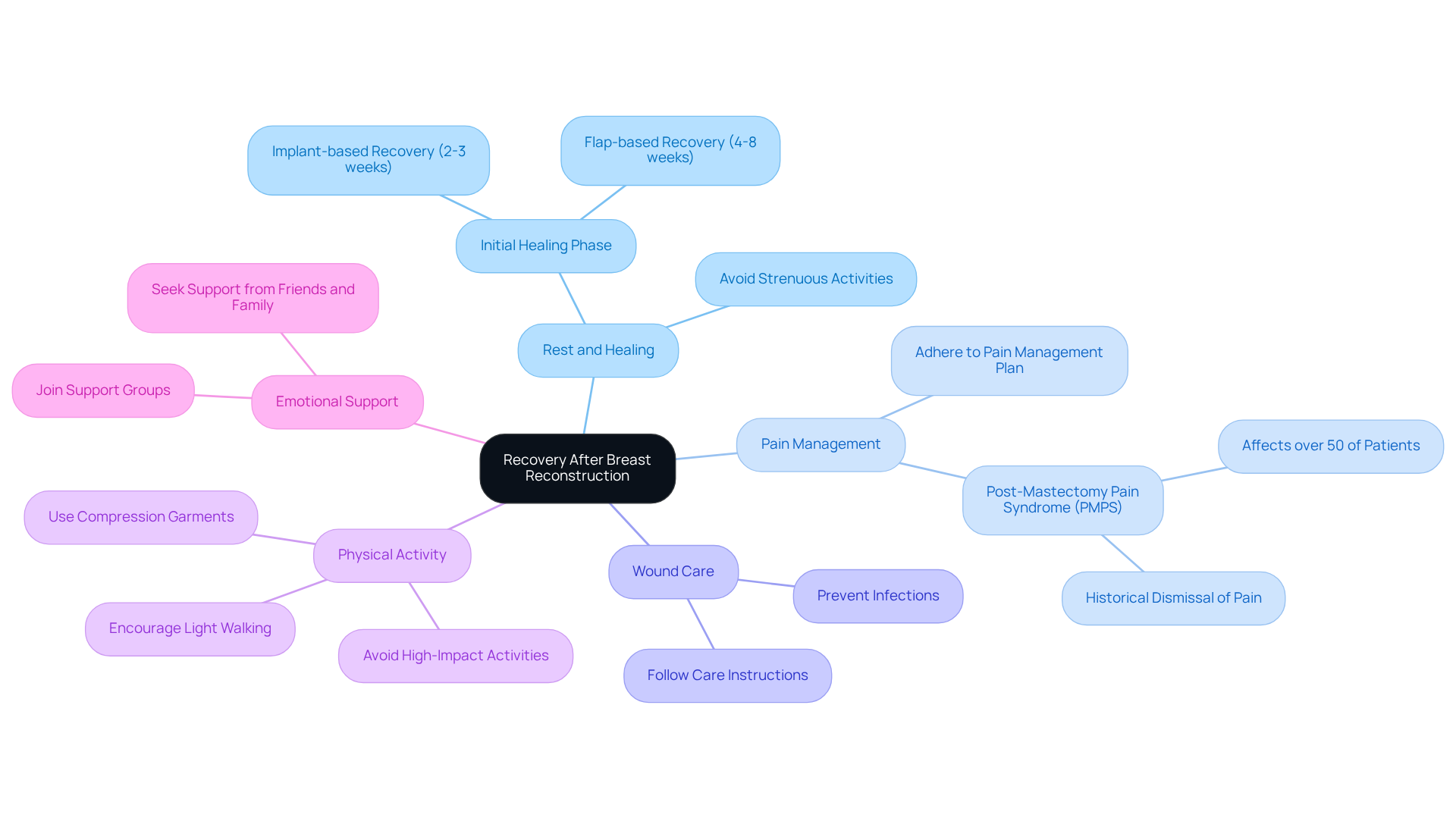
- Rest and Healing: In the initial healing phase, which typically lasts between 2 to 8 weeks depending on the procedure, prioritizing rest becomes paramount. For those undergoing implant-based reconstruction, a recovery period of approximately 2 to 3 weeks is anticipated, while flap-based reconstruction may necessitate 4 to 8 weeks, alongside additional healing time for the donor site. It is essential to avoid strenuous activities and heavy lifting, as this minimizes complications and fosters a smoother healing process.
- Pain Management: Post-surgery pain and discomfort are common companions on this path. Adhering to the surgeon’s pain management plan, which may encompass prescribed medications and over-the-counter options, is crucial. Notably, research indicates that post-mastectomy pain syndrome (PMPS) affects over 50% of individuals undergoing mastectomy, a reality recognized since the 1970s. This underscores the necessity for effective pain management strategies. As plastic surgeon Maureen Beederman eloquently states, “A surgery should only be deemed successful if the individual is pain-free.”
- Wound Care: The integrity of the surgical site is vital for preventing infections. Patients must diligently follow the specific care instructions provided by their healthcare team to ensure optimal healing. Dr. Golshani emphasizes the importance of adhering to post-care instructions, which can maximize results and minimize risks, guiding patients toward a successful recovery.
- Physical Activity: Light walking is encouraged to enhance circulation, yet patients should refrain from high-impact activities until receiving clearance from their surgeon. Gradually reintroducing physical activity can assist in recuperation while avoiding strain on healing tissues. Compression garments or bandages may also be fitted to support healing and minimize swelling, further aiding the recovery process.
- Emotional Support: The emotional toll of healing can be profound. Seeking support from friends, family, or support groups can be invaluable. Many individuals, like Jeni Golomb, who relies on gabapentin for chronic pain management, find solace in connecting with others who have faced similar experiences. This connection can alleviate feelings of isolation and provide essential support. Dr. Golshani’s empathetic approach ensures that individuals feel nurtured throughout their healing journey.
By understanding these recovery expectations and strategies, patients can better prepare for their healing journey, focusing on their overall well-being and embracing the transformation that lies ahead.
Conclusion
Breast reconstruction following a mastectomy is not merely a medical procedure; it is a pivotal chapter in the journey of reclaiming one’s identity and emotional well-being. This transformative process transcends physical restoration, nurturing a renewed sense of self and confidence. By exploring the array of reconstruction options available, individuals can embark on a path that resonates with their personal aspirations, ultimately enhancing their quality of life.
This article illuminates the profound significance of breast reconstruction, shedding light on the psychological benefits it bestows. With a focus on both implant-based and tissue flap reconstruction methods, it thoughtfully outlines the advantages and considerations of each, offering a comprehensive understanding of the choices at hand. The emphasis on preoperative consultations, the surgical journey, and recovery strategies underscores the necessity for informed decision-making and active engagement in one’s care.
Ultimately, the journey of breast reconstruction stands as a testament to resilience and empowerment. It invites individuals to engage in candid discussions with their healthcare providers, explore the latest advancements in techniques, and prioritize their emotional health throughout this significant process. Embracing this transformative experience can lead to remarkable enhancements in both physical appearance and mental well-being, highlighting the essential role of reconstruction in the lives of those navigating the aftermath of a mastectomy.
Frequently Asked Questions
Why is breast reconstruction after mastectomy important?
Breast reconstruction is important as it helps individuals reclaim both the physical beauty of their chest and their emotional well-being, allowing them to rediscover their sense of wholeness and femininity, ultimately rebuilding their confidence.
What psychological challenges do women face after a mastectomy?
Many women experience profound psychological challenges, including feelings of loss and diminished self-esteem, which can significantly impact their emotional stability and quality of life.
What percentage of women report improvements in body image after breast reconstruction?
Approximately 76% of women who undergo breast reconstruction report significant enhancements in body image and overall quality of life.
How does the timing of breast reconstruction affect emotional recovery?
The timing of reconstruction, whether immediate or delayed, plays a critical role in emotional recovery, with immediate reconstruction being associated with superior emotional outcomes and reduced feelings of distress.
What advanced techniques does Dr. Golshani use in breast reconstruction?
Dr. Golshani employs advanced techniques such as the Keller Funnel and the no-touch technique to ensure safe and efficient procedures that minimize risks and enhance recovery.
What is the importance of personalized care during consultations?
Personalized care during consultations is crucial as it allows Dr. Golshani to listen attentively to patients’ aesthetic aspirations and concerns, fostering a nurturing environment that supports recovery and reassurance.
What factors should patients discuss with their healthcare providers regarding reconstruction options?
Patients should address specific issues such as breastfeeding after augmentation and the pros and cons of implant placement, as these factors significantly influence the decision-making process for reconstruction options.
What do testimonials from patients indicate about Dr. Golshani’s practice?
Testimonials indicate that Dr. Golshani’s practice is viewed as a sanctuary, highlighting the nurturing environment that fosters recovery and reassurance for patients undergoing breast reconstruction.
List of Sources
- Explore the Importance of Breast Reconstruction After Mastectomy
- Impact of breast reconstruction on quality of life among women after mastectomy – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC12799536)
- Immediate Breast Reconstruction Reduces Psychological Impact of Mastectomy (https://wolterskluwer.com/en/news/immediate-breast-reconstruction-reduces-psychological-impact-of-mastectomy)
- Rates of breast reconstruction after mastectomy have stabilized (https://wolterskluwer.com/en/news/rates-of-breast-reconstruction-after-mastectomy-have-stabilized)
- Health Legislation Update Brings Breast Cancer Care Into the Modern Age (https://plasticsurgery.org/news/press-releases/health-legislation-update-brings-breast-cancer-care-into-the-modern-age)
- ‘I just want to feel like me again’: the women still waiting for breast reconstruction years after lockdown (https://theguardian.com/society/2026/apr/13/i-just-want-to-feel-like-me-again-the-women-still-waiting-for-breast-reconstruction-years-after-lockdown)
- Examine Types of Breast Reconstruction: Implants vs. Tissue Flaps
- The breast reconstruction journey: What’s changed since 1998? (https://plasticsurgery.org/news/articles/the-breast-reconstruction-journey-whats-changed-since-1998)
- Safer, lasting breast reconstruction via tissue flap surgery – WellSpan (https://macroscope.wellspan.org/news/safer-lasting-breast-reconstruction-via-tissue-flap-surgery)
- Implant vs. Flap Breast Reconstruction Surgery: How To Decide | Memorial Sloan Kettering Cancer Center (https://mskcc.org/news/breast-reconstruction-deciding-between-implant-and-flap-surgery)
- Why DIEP Flap Is the Gold Standard in Breast Reconstruction (https://prma-enhance.com/blog/diep-flap-continues-to-be-gold-standard)
- Understand the Steps Involved in the Breast Reconstruction Process
- New Breast Reconstruction Research Expands Patient Options (https://breastadvocateapp.com/2026/02/15/new-research-shows-promising-innovations-in-breast-reconstruction)
- New plastic surgery statistics and breast reconstruction trends (https://plasticsurgery.org/news/blog/new-plastic-surgery-statistics-and-breast-reconstruction-trends)
- New Legislation Advances Breast Cancer Care into Modern Age (https://facs.org/for-medical-professionals/news-publications/news-and-articles/bulletin/2026/april-2026-volume-111-issue-443/new-legislation-advances-breast-cancer-care-into-modern-age)
- New 1-day surgery removes cancer and reconstructs the breast in the same operation (https://abcnews.com/US/new-1-day-surgery-removes-cancer-reconstructs-breast/story?id=126492962)
- Navigate Recovery After Breast Reconstruction: Tips and Expectations
- Breast Cancer Survivors Face Debilitating Post-Mastectomy Pain – NYC Today (https://nationaltoday.com/us/ny/new-york/news/2026/04/11/breast-cancer-survivors-face-debilitating-post-mastectomy-pain)
- These women had their breasts removed to thwart cancer. Then came the pain. | CNN (https://cnn.com/2026/04/11/health/mastectomy-breast-cancer-pain)
- Mastectomy Patients Struggle With Chronic Pain After Surgery – Chicago Today (https://nationaltoday.com/us/il/chicago/news/2026/04/06/mastectomy-patients-struggle-with-chronic-pain-after-surgery)
- Breast Cancer Survivors Face Years of Post-Surgery Pain (https://goodmorningamerica.com/wellness/story/pain-persists-breast-cancer-surgery-9047563)
- Low Food Access May Lead to More Complications After Breast Reconstruction (https://ascopost.com/news/april-2026/low-food-access-may-lead-to-more-complications-after-breast-reconstruction)

